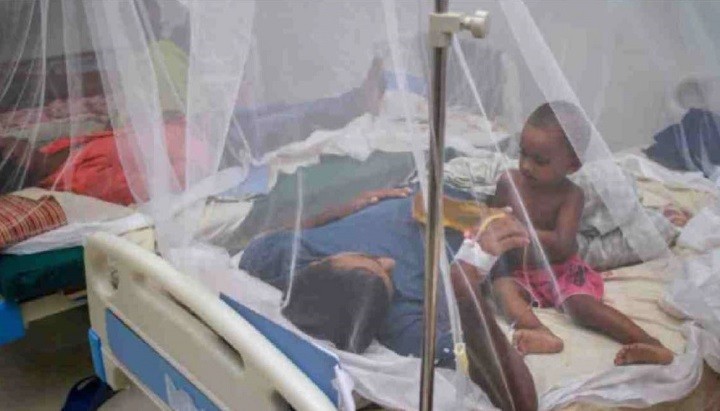
Covid-19 may no longer be a serious health threat to
Bangladesh as the country has already achieved herd immunity against the virus
with the widespread infections of the highly transmissible Omicron variant, say
experts.
Though there is no credible study and serosurvilnce report
here to know about the immunity developed among people across Bangladesh, the
medical analysts think the virulent Omicron acted like a natural vaccine
infecting most population in the country, helping build the herd immunity.
Talking to UNB, leading public health experts Dr Bijon Kumar
Sil, Prof Muzaherul Huq and Dr Be-Nazir Ahmed said any new variant of the virus
can still infect people having the immunity gained through the Omicron
infections, but it may not cause severe illness.
They, however, warned that any type of Covid variant can be
dangerous for only the immunocompromised people and those who have
comorbidities.
Herd immunity is a concept based on the body's immune
resistance to the spread of a deadly disease (bacterial or viral infection) and
it can be obtained in two ways -- naturally through infections of the majority
of the population and artificially through vaccinating around 80 percent of the
population of a country.
High-quality immunity
Dr Bijon Kumar Sil, head of the microbiology department at
Gono University, said the way Omicron has spread across Bangladesh, leaving
behind a high-quality natural immunity among people in the country. “So, I
think Covid may not cause serious problems in the country in the days to come.”
He believes Bangladesh has already attained herd immunity
like many other countries in the world.
“It’s very good quality herd immunity. Natural herd immunity
is much better than vaccine-induced immunity. The American CDC is also now
recognising the natural immunity gained through Omicron infection is as good as
double or triple vaccinations,” the expert said.
He said not only Bangladesh but also many countries in the
world are going to attain natural herd immunity because of massive exposure to
the Omicron variant. “As Omicron has spread rapidly all over the world, hardly
anyone will remain without a natural antibody with the ebbing of its wave.”
Dr Bijon thinks over 80 percent of people in Bangladesh have
already been infected by Omicron, while over 70 percent have already received
the first dose of vaccines. “So, the new variant in the future is unlikely to
cause any big problem in terms of severity of the illness.”
Dr Be-Nazir Ahmed, former director (disease control) of
DGHS, said Omicron worked as a natural vaccine as most people of the country
were infected by it. “So, we’ve already gained the herd immunity against the
Covid virus.”
He said the new normal life will not be affected and people
may not suffer much from the Covid if any new variant does not come that can
dodge the existing immunity of people.
Going to be like flu
Dr Bijon is hopeful that Covid-19 will become like a flu in
the near future, but it will not be eliminated from the world. “If a new
variant emerges in the coming days, it may infect people with symptoms like
many other remaining flues.”
He, however, said new variants are likely to be a matter of
concern for the people who are immunocompromised.
Dr Bijon said the massive surge in omicron cases all over
the world is signalling the beginning of Covid’s transition to become endemic.
“The World Health Organisation may declare Covid as endemic within six months
if any unusual variant does not emerge.”
Conducting studies
Bijon said the government should immediately conduct a
countrywide serosurveillance to know how many people gained natural antibodies
through Omicron infections and also to know the comparative performances and
the longevity of antibodies produced by the different vaccines and natural
infections.
He said such a study will help upgrade the ongoing
vaccination drive and ensure the scientific and effective use of the jabs.
“Most countries in the world are now conducting
serosurveillance to know whom they should now vaccinate after the Omicron wave.
We should also do it.”
Echoing Bijon, Dr Be-Nazir said the studies are also
necessary to know in which cities and districts the antibodies are much more
among people and where less among them.
“We should also know which types of people have low
immunity. If we can know this, we’ll be able to intervene in the areas where
people have low immunity. It’ll also help redesign the mass vaccination drive,”
the expert said.
Besides, he said, the government should take steps for
various studies on Covid to know the real situation in the country and work out
future plans based on scientific data.
Necessity of vaccines
Prof Muzaherul Huq, a former adviser to WHO (South-East Asia
region), said Bangladesh surely achieved the herd immunity with the extensive
infections of Omicron.
“But herd immunity is now not a big factor as we still have
to provide our 100 percent people, including the children, with the vaccines as
we aren’t sure about how durable this immunity would be or how well it would
work if a different type of Covid strain emerges in the future,” he observed.
Dr Huq said it is sure that Covid will not disappear from
the world soon as its different variants, even the old ones, will remain and
continue to infect people. “So, we shouldn’t depend on herd immunity. Rather,
we should count on vaccines to keep us protected from the virus.”
He said even the virus infection rate can come down to below
one percent in Bangladesh within months, but it may increase further anytime
with the emergence of any new virulent variant.
“So, people should continue to wear masks and maintain
health safety rules alongside receiving vaccines,” the expert advised.
He said vaccine companies are carrying out research to
improve the quality of their existing jabs. “We may get an effective vaccine in
the near future which will give us life-term protection against the Covid
virus. Until we get such a vaccine, we need to continue the vaccination drive
and ensure booster doses for all.”
Dr Bijon, however, said people who have taken two doses of
vaccines and get infected with Omicron may not require the booster dose.
“The people who got infected with Omicron, except those
having comorbidities, may have strong immunity as Omicron replaced all the
previous variants,” he opined.
-
UNB